Peter was born on the 13th January 1987 at the City Hospital in Birmingham, the second eldest child of a family of what was
to be four children.
After a long period of labour he was delivered naturally, but indications from the staff implied
something was not quite right.
The cord was wrapped around baby's neck. Both Mom and Dad overheard the mention of phoeatal
distress. Within a few moments a pediatrician was called and by this time there were more staff in the labour ward.
Peter was taken straight from Mom.
Dad noticed that baby looked a bluish colour and was not making any sound or movement,
he was placed on a piece of equipment and the staff acted with some urgency in doing what they did,
it was a very distressing few minutes as both mom and dad looked on wondering what was happening,
then came a little cry and baby was seen to move, both Mom and Dad were filled with emotion at the relief
of hearing him overcome what was to be his first hurdle in life.
The first born to the family was a girl,
Cheryl who was found to have a heart condition, as a result of this, when the doctor came on his rounds,
Mom asked if he would check Peter's heart to make sure all was well, and was told by the Doctor that everything was fine.
The next day Mom popped to the bathroom to wash, leaving baby asleep at the side of her bed, but upon returning saw
that baby had gone, she immediately enquired as to where Peter was and was told that he had been taken to another
room by a Doctor and was having his heart checked. Mom waited anxiously for their return.
When the doctor came back he told Mom that Peter
had been diagnosed as having a heart murmur and would eventually be referred to another Hospital.
After their discharge from the maternity unit. Peter's next appointment was at Good Hope Hospital, Birmingham,
where it came to light that Peter had a V. S.D (Ventricular Septal Defect) a hole in the heart,
and was not seen again until 1991 after a further referral to Birmingham Childrens Hospital.
After undergoing some tests and seeing the Cardiologist, Peter was diagnosed as having
mild pulmonary stenosis; a follow up appointment was made but was not until 1993.
At the appointment in 1993, the same cardiologist saw Peter and after tests were told that his condition remained the same
(mild Pulmonary Stenosis), a further appointment was made for Peter to be seen in 1996.
1996... at this hospital visit Peter was seen by one of the registrars who after viewing the test results, told Mom that Peter's
condition had become worse and now had a problem with the left side of the heart and would need to be seen annually,
after enquiring what was wrong, Mom was told that Peter had aortic Stenosis and aortic regurgitation, Mom asked how he had
developed this and was told that it was due to his Pulmonary Stenosis and that the left side was helping the right side of
the heart, this statement was accepted as at this time all the medical terminology was completely above mom and dads heads.
As the year went by Peter had been having Asthma type symptoms and had lost a lot of time from school, he regularly went in and out
of hospital to be treated for his breathlessness and was taking steroids and inhalers to relieve the effects.
In 1997 Mom and Dad took Peter to his appointment where he had Echo and E.C.G
tests and afterwards waited to see his regular cardiologist, during this
time Peter's records were placed outside the examination room ready for the cardiologist
to view and evaluate Peter's latest
conditions.
After a long waiting period Mom, Dad and Peter were called into the examination room,
there were other student doctors in attendance, the cardiologist placed Peter's records
on a desk and did not refer to them at any time, instead he and his students made a physical examination while talking technically
to each other, at the end of the examination Mom
and Dad were told that Peter only had Pulmonary stenosis and would not need to be seen for
a further 18 months.
Mom immediately questioned this diagnosis and pointed out the previous years results from the registrar, she was again
told that Peter had pulmonary stenosis and he would be seen again in 18 months time.
Dad was delighted in his ignorance that Peter's condition was not as serious as explained
the previous year, Mom however felt very uneasy and decided to follow up her suspicions by visiting the family G.P
on the same day, the G.P wrote a letter to the hospital relaying mom's anxiety, its contents contained a statement which
included a comment saying " 1 don't know where mother is coming from, as our records show that there is only a problem
with the pulmonary valve."
The G.P received a reply from the hospital and mom went to the surgery where she was told that Peter
had got problems with his aortic valve, as well as his pulmonary valve, she asked if
Peter would be alright for 18 months or will he need to be seen sooner, the G.P said
he should be fine.
In 1998 Peter was rushed into another Hospital with severe asthma symptoms where
he was seen by a Doctor who specializes in this condition and after examining Peter wrote a letter to the Childrens hospital stating 'I do not think the Asthma
is related to his heart condition, but please could you tell me what is wrong with this boys heart."
The Doctor received a reply from the Cardiologist saying Peter has only got pulmonary stenosis.
Peter was seen in 1999 by his Cardiologist, he done his tests on him and then called
them into a room and told Mom and Dad that Peter's pulmonary valve would need balloon dilation
sometime that year, after several cancellations Peter was finally admitted
in January 2000 for the above procedure.
Prior to going to the theatre Dad signed a consent form and Peter, Mom and Dad went to
the pre operating room where Peter was to be sedated, seconds before Peter was put to sleep Mom and Dad were asked to sign another
consent form to allow another procedure to be carried out, this distressed both parents who questioned why, they were told that
a T.O.E (Trans oesophical echocardiogram) needed to be performed so the back of the heart could be seen in more detail,
this raised suspicions as to why it was not discussed or explained prior to this time.
The procedure was carried out and Peter
was returned to the ward. Later that day the cardiologist came to see the Family, he said the ballooning of the pulmonary valve
was successful but ... (Mom looked straight at him with great concern) he had found a small piece of skin below the aortic valve,
Mom asked, would Peter need open heart surgery, then came the bombshell answer which was yes, within the next few months.
This devastated all concerned because the severity was never explained to the Family. Mom fired a series of questions to the
Cardiologist asking what this small piece of skin was he explained that it was normally found in young children who have a
hole in the heart.
Peter had suffered for years with chest pains, leg pains, tiredness, lack of concentration,
breathlessness and quite often had a bluish tinge to his lips but a few months later, in April, Peter
developed severe symptoms which included all the above but they
were more severe, he was taken straight to the Childrens hospital ward where he was seen by one of his normal cardiologists
understudies, he listened to what Mom and Dad had to say and then checked Peter over,
he made notes on a piece of paper because Peter's records were not available at that time,
he then said that Peter needs open heart surgery soon and will be in touch.
The family returned home. Four weeks went by and a telephone call was received from the hospital for Peter
to be admitted, his hospital bag was packed and was taken to the hospital ward in preparation for this major operation,
the surgeon came to see the Family and a consent form was signed by Dad.
The surgeon told them Peter would be prepared for theatre and also stated, as
well as a resection of this small piece of skin he may well need an aortic valve replacement as he is not sure how much damage had
been caused, Mom questioned the surgeon and asked what is this small piece of skin, to which he explained it to be a membrane with
roots. More Doctors turned up to examine Peter to see if he was fit enough for surgery,
but unfortunately the operation had to be cancelled because Peter had a cold.
Mom and Dad took Peter home. Peter
was readmitted and on the 19/5/2000 was taken to theatre for
his operation that was expected to take four hours, he was anaesthetized and Mom and Dad kissed him and battled to hide their
emotions.
They were not asked to sign another consent form. Six long hours went by, Mom and Dad grew more and more anxious as
it was taking so much longer than anticipated so Dad went to the intensive care unit to see what was happening, at that very
moment Peter was being wheeled into the I.C unit surrounded by a large amount of hospital staff,
it was a very distressing sight, with all those pipes and wires coming from his body.
A Doctor spoke to Dad as Peter was being connected to the various equipment but
Dad cannot to this day recall a word of what was said to him. Dad returned to Mom. to give her the news, by this time she was in
the corridor, tears were rolling down her face and was panicking to hear how her son was, she dried away the tears took a deep
breath and prepared herself for what she was about to encounter. Peter spent that night and most of the next day in the I.C Unit
and was then well enough to be moved back to the ward.
The surgeon who performed the operation popped in to see Peter and said the
surgery was a success but this membrane has a 5% chance of recurring, he then left. Mom and Dad were so concerned about their son
that they put off asking any questions fill later. Several requests to see the surgeon were made by Mom and Dad during Peter's stay,
but he never came. As Peter was becoming better, he was being weaned of the pipes and tubes that were attached to him one of these
being a pericardial drain that was inserted via his lower chest, shortly afterwards Peter became unwell and it was decided that
the drain pipe would need to be re-inserted to drain off a build up of excess fluid, this involved going back to theatre and
signing another consent form, Peter was starting to have enough and began to cry, but like the brave boy that he proved to be,
endured the additional pain, he was then returned to his bed in the ward. Peter made a good recovery and was discharged on the
28/5/2000, he was very pleased as this was his little sister birthday and he could go to her party.
Mom was not at all happy that the surgeon did not come to see her to answer a build up of questions that she had unanswered, so
decided to do her own research into what exactly Peter's past and future held. She began by seeing the Family G.P who told her that
Peter's condition was called D.M.S.S (Discrete Membrane Subaortic Stenosis) from here a request to view Peter's
medical records was made to the hospital.
Whilst viewing the records even more questions came to mind and a complex list of various details that were
never mentioned or discussed with the family was made so further information could found. Next came the painstaking visits to the
main library and the university library, studying medical journals and surfing the Internet for as much information as possible
and the more that was discovered, the greater the concern for Peter's future became. Mom and Dad began to feel that their son had
not received the correct medical treatment to correct his conditions and began to lose faith in the N.H. S system.
By chance Mom was on the computer hoping to find out more about Peter's conditions
and happened upon Miami Childrens Hospital website, it contained a vast amount of details about surgeons,
operative procedures and performance statistics, they seemed perfect to
contact about Peter's conditions.
Contact was made by telephone to the Cardiac unit at Miami Childrens Hospital where Mom
expressed her concerns, they were very helpful and a few telephone calls later Mom spoke personally to the surgeon who has
had experience of Peter's conditions and suggested that
Peter's E.C.G's be sent over to them for evaluation, or to bring him
personally.
It is now late May 2001, Peter was again unwell and was showing the same symptoms prior
to his first open heart surgery, a telephone call was made to the ward at the Childrens hospital and Mom explained what was wrong,
to her astonishment she was told that they were too busy to see Peter.
Peter began to get worse so Mom took him to the heart unit at the childrens hospital where he
was placed on an E.C.G and Echo machine by a different Cardiologist, Mom asked how Peter
was and was told that his pulmonary valve was leaking, when enquiries were made about the membrane,
it was stated that the growth was no longer present, Mom knew in her heart that something was not right, Not
at all happy with these results Mom and Dad spoke with each other and decided the best thing would be to take Peter to Miami.
The next hurdle was obtaining the finances to cover the costs of the flights, accommodation, the evaluation fee and living expenses.
Fortunately Peter's Grandmother offered to lend the money.
A telephone call was made to Miami Childrens Hospital, an appointment date was made for July 23rd 2001 and the
only flight available was from Manchester airport to Sanford Orlando, in the north of
Florida, so a flydrive booking was arranged for July 19th 2001.
Arrangements had to be made for Peter's sisters to be looked
after for the following 8 days while Mom Dad and Peter made the journey.
After hours and hours of traveling, getting lost a few times and spending a couple of nights in a hotel, it was time for
Peter's appointment at Miami Childrens hospital.
On the Monday morning, after going through the registration process, the family where made extremely welcome at the cardiac
co-ordination reception and were directed to various departments of the hospital for tests,
Peter had an E.C.G, chest x-rays and an E.K.G prior to meeting
a cardiologist for a physical examination, all this information was presented and the case discussed at a conference
meeting the following day by the Cardiac team.
An appointment was made for the Wednesday to meet with the surgeon to discuss the situation.
Mom, Dad and Peter met with Dr Redmond Burke, the surgeon,
who explained in great detail what was wrong with Peter and what was required,
the membrane that was reportedly resected successfully during the first open heart surgery was still there and is creating
further damage.
Dr Burke came across as a very capable, caring and honest man, he pulled no punches and stated that unfortunately
Peter had fell into a crack in the pavement, and the past cannot be changed but he
could do something for the future. Mom asked if she would lose Peter,
Dr Burke assured her that Peter would be O.K but would need a "Konno Procedure"
with a prosthetic aortic valve sometime within the next 12 months.
He explained that he had performed this procedure several times before without losing a patient, he said he
could do the operation now but it would be better for the surgeon and patient to wait a while, because of the scar tissue being
so new, he offered to watch Peter's future progress during this period,
which at this time was described as being moderate to severe.
It was now clear what was wrong with Peter and what was needed to keep him alive.
The "Konno procedure" involved cutting a section of heart muscle away to gain access into the heart,
doing what is necessary then replacing this with a patch.
Dr Burke clearly had the experience and expertise to perform such a task. The life saving treatment
Peter required was classed as a level 1, and under an international
heart package would cost $50,000. The journey home was made and on returning issues were raised with the Childrens Hospital who had
previously treated Peter. Several meetings were held with various hospital staff as to Peter's past and future treatment but it all
seemed to be a vicious circle.
A request was made to change cardiologists as the family felt Peter had been let down in the past.
Mom and Dad decided that Peter would be best treated by Dr Burke and wrote a letter
to the Prime Minister, Tony Blair, and requested that the N.H.S fund the operational costs in America,
he in turn put the case in the hands of the Regional Health Authority.
The Regional Health Authority made their enquiries to the Childrens Hospital and they then contacted
Peter's Mom stating that as a result the "Konno" was not the preferred option for
Peter and alternative treatment was on offer, this lead to an appointment
to see a surgeon at Great Ormond Street Hospital.
Funding for America was refused, they said that Peter did not fit the criteria.
On the Saturday prior to the following Fridays visit to London, Mom received a telephone call from the surgeon at Great Ormond
Street, who in no uncertain terms told mom that they no longer performed the "Konno" that
Peter needed and if it was attempted, he probably would not make it through the operation,
this news frightened Peter's parents and upset them tremendously.
The Friday came and the Family attended Great Ormond Street Hospital where Peter
had tests before meeting with the surgeon, he explained that further resection of the membrane could be done but
Peter does not need an operation, and his condition
is only mild, he continued and said at some stage in Peter's life he will probably need surgery.
When asked how many times a membrane resection could be carried out on a single patient,
Mom and Dad were told that he had done this ten times on one patient, they found this all too much to comprehend and left at the
end of the meeting feeling very confused as to the vast difference in opinions between America and the U.K. One must be right.
The availability of the "Konno" in the U.K was the next task to investigate.
In the meantime attempts to raise the funds were being made but with very little response. A reporter from the local newspaper
became interested and made a visit to the family home, listened to the story so far, and began to make his own enquiries into
the medical statistics surrounding the "Konno". Within a few days the reporter had been in touch with several hospitals
throughout the U.K and spoke with the Royal College of Surgeons, the "Konno" had only been performed 5 times,
3 patients had died and there was no information available on the remaining 2.
The statistics were shocking. Peter's new cardiologist stated that in the past,
mistakes, errors and wrong decisions were made with Peter and he was in agreement with
the report from America.
Peter's condition is moderate to severe.
This strengthened the family's case to get the funding from the Regional Health
Authority. It was now March 2002. Results taken from the Birmingham Childrens Hospital were sent to
Dr Burke at Miami Childrens
Hospital and time was becoming a major concern, Peter was getting worse.
Several phone calls to the Regional Health Authority
stating the new evidence were made, but their decision remained unchanged.
Mom, and Dad refused to give up the fight to save
their son and tried desperately to arrange fund raising events, car washes at the local fire station, raffles, approaching
various registered charities and having an appeal placed in the Birmingham evening Mail, very little was raised and the target
figure seemed impossible to achieve.
In a desperate attempt Dad sent out over 200 emails to people and organizations in the
hope someone would help, out of all the negative responses there was an email reply from the secretary to Alan Milburn M.P
saying Dr Roger Boyle (National Heart Director) was looking into the matter, and another which looked promising was from the B.B. C health correspondent, a man
called Michele Paduano. He was interested in what was happening and arranged a date for an interview.
A short while later a preliminary interview was held at the family home to gain some background information about what had gone
on and the validity of the story. Michele then organized a televised interview to take place within the next few days.
The television crew turned up in the morning and the nervous parents did their best to highlight their plight. All went well.
The crew then rushed off to get a
statement from a spokesperson for the Regional Health Authority and try to get the story ready for the lunchtime edition of B.B.C
Midlands Today.
Michele telephoned Mom and Dad saying that he could not get the statement from them until after the deadline for
lunchtime, but told them to watch the early evening news at 6.30pm.
The family gathered round the T.V and to their astonishment
a satellite link to Dr Burke in Miami was included, Dr Burke explained the "Konno procedure"
Peter needed and clearly stated that
the need for surgery soon, outweighed the risks involved. Mom and Dad thought that this must prove, that taking into account the
availability of the "Konno" and the alternative treatment that was being offered to Peter
in the UK, justified funding for a once and for all operation in America.
A letter was sent to the Regional Health Authority from Peter's parents respectfully
requesting that they review Peter's case and
change their decision, as surely Peter does fit the criteria for overseas funding.
Mom came across a charity that offered wishes to
sick children, they were called Purple Dreams and are based in Wolverhampton, mom spoke with them over the telephone and they sent
some forms out to be filled in with the request details.
This was done and the section, which asked what was wanted, was replied to
with a request for Peter to have his operation performed by Dr Burke in America.
Dad drove to Wolverhampton and personally handed back
the forms for consideration, the staff were amazed at the request and stated they had never had a request for this kind of thing
before but would certainly look at it during a meeting with their board the next day. The situation was becoming desperate, waiting
for replies, making no progress, just hoping a miracle would happen.
The lack of communication leads Mom to contact Dr Roger Boyle personally, which she did. She wanted to make sure that he
was aware of
all the facts and what was being done to resolve the situation, it was a good job she did, the information that he had was not correct,
he had been told that Peter's condition was only mild.
Mom argued to the contrary and insisted that Peter's condition was moderate
to severe and that the cardiologist at Birmingham Childrens hospital can confirm this. Dr Boyle suggested that a further opinion
be sought from another hospital in Newcastle and could arrange this within 48 hours.
Having no choice, Mom and Dad agreed and Dr Boyle said he would get back in touch.
In the meantime an appointment at Birmingham Childrens Hospital was due and the family
attended, this appointment was most important as it could save journeying around the U.K to prove the severity of
Peter's condition.
The cardiologist agreed that Peter's condition was moderate to severe. With this information
Mom immediately telephoned Dr Boyle and explained the results. Dr Boyle said he would Phone the cardiologist
straight away to confirm the situation, within the hour Dr Boyle was back in contact with Mom, he said he had spoken
with the cardiologist and you are right, Peter's condition has
been confirmed as moderate to severe, he had also been in contact with the Regional Health Authority and that they would be in
touch soon, Mom asked how soon, the reply was, very soon.
Within the hour the telephone rang, Mom answered, it was the Regional
Health Authority, Dad watched mom's response eagerly, mom was filled with emotion and said please explain this to my husband
and passed the phone to him. Dad listened to the following statement...
we apologize for what has happened, it is not our fault,
the previous decision was made based upon the information we had received from the hospitals involved, and as a result,
we agree that Peter fits the criteria for overseas funding, and to carry on and make the
necessary arrangements. Dad replied this is fantastic news,
1 hope this will help other children in the future. The reply was.... fortunately there aren't many
Peter's in the world.
Mom asked for the decision in writing, which was agreed and mom was assured that no one would change this
decision. Words cannot express the tremendous relief that was felt by the family. Peter now
had a fighting chance.
As a result of the wonderful news, Mom began making telephone calls to relay the good news. The B.B.C were informed,
returned and televised the updated story, Purple Dreams were contacted with the news but still insisted that they do
something for Peter and agreed to arrange and pay for the airfares, this was great because this
time they could go as a family.
It is now early July 2002, Mom contacted Miami and Peter was booked in for the
29th July 2002 for tests and the 31st July for
open-heart surgery.
The flights, were arranged for the 23rd July 2002 from Gatwick Airport direct to Miami International Airport,
all looked set, but just as things seemed to be going well, another hurdle appeared, it was to do with insurance to cover Peter
in the event things did not go as planned.
One quote was given but would cost £39,000; no one seemed to want to take
on the risks.
This problem was eventually overcome when the Regional Health Authority agreed to use their own insurance and
in the event of anything happening would cover any additional costs themselves.
The funds which were raised previously,
what the family managed to save, and a personal loan amounted to £4,000 this was to be used on travel expenses from
Birmingham to Gatwick return, travel, accommodation and living expenses for the unknown amount of time to be spent in America.
The family arrived at Miami on the 23rd July 2002 and found accommodation for the next 6 days prior to the hospital apartment
being available. Peter was coping well with the thought of what was to come. The 29th soon came
round and Peter was
registered prior to having all the tests that he was well used to by now. The results were gathered and a meeting with Dr Zackheim,
(the cardiologist) took place.
Details about Peter's forthcoming operation
were discussed. Peter was allowed back to the hospital apartment.
The big day had arrived (Wednesday 31st July 2002) and all
the family attended the hospital at 6am in the morning, mom, dad and Peter went into the pre
operative ward where Peter was to
be sedated prior to his surgery.
Peter put on his hospital gown and lay on the trolley
looking continuously at mom and dad.
Members of the cardiac team gathered around and Peter was given a sedative by mouth,
which would take effect within a few minutes.
Dad tried to take Pete's mind of things by betting that he would be asleep within the next five minutes.
Peter continued to stare
at mom and dad and within five minutes had closed his eyes, then, within a few seconds sat up and said ha ha you've lost your bet
dad.
A few minutes later Peter was out for the count and mom and dad kissed him before he was
wheeled away into theatre and yet
again tried to hide their emotions. Dr Burke came to see mom and dad before the operation and told them that they would be
informed at least every half hour as to how things were progressing and would speak to them again after the operation.
The procedure started at about 7am. The hours went by and the family was kept informed continuously by one of the cardiac
nurses who was in and out of theatre with the latest news. Mom and dad were so anxious and concerned they would look for the
expression on the nurses face as she walked towards them along the corridor as an indication as to how things were.
Midday came and the latest news was that Dr Burke had now entered into the heart, had removed the membrane,
the unrepairable aortic valve and was preparing to insert the prosthetic aortic valve.
Peter was coping well.
By late afternoon news came that Peter was being weaned off the bypass machine but
had to be shocked to start his heart, they were told not to worry as this was often the case under these circumstances.
The waiting continued, then, at about 5 o'clock Mom looked to her left and saw Dr Burke walking towards them,
he had a big beaming grin on his face which spoke a thousand words, he said straight away that Peter
was doing marvelously. Mom started crying and threw her arms around him, dad shook his hand and they thanked him continuously.
In his hand, Dr Burke held a series of photographs,
which had been taken throughout the operation, there were 17 in total, he used them to explain and show mom and dad exactly what
had been done. He went on to say that he did not know why there were so many incisions made around the aortic valve from the
previous operation and that you would not want the same people doing this again, he added you made the right decision to bring
him and told mom she was one hell of a mother.
Peter had the "Konno", a 21mm prosthetic aortic valve, his pulmonary valve had
been repaired, the aorta had been doubled in size and over 400 stitches used in his heart.
Dr Burke had rebuilt Peter's heart,
it took him 10 hours. He truly is a miracle worker. Shortly after, Peter was taken from
theatre to the intensive care unit.
Mom and dad went in to see him; he looked good considering what he had endured.
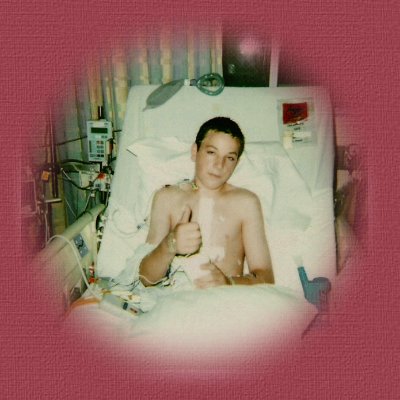 Taken at Miami Childrens Hospital Day after operation (1st August 2002)
Taken at Miami Childrens Hospital Day after operation (1st August 2002)
Peter's sisters came in to see him but found
it too distressing; they both began to cry at what they saw.
During that evening Peter was monitored closely one to one by the
I.C nurse, he had his eyes open and was quite alert throughout the night.
Early the next day, Peter looked at mom and lifted
his hand to touch his lips, he wanted a kiss, he then said, "I'm a lucky boy to have a mom and dad like you
". As the hours went
by Peter became more aware and was well enough to have some of the pipes wires and tubes removed,
he even managed to change his boxer shorts himself.
The following day Peter was now out of bed and walking around the I.C ward,
he was now making a fantastic recovery; the Doctors were amazed, they called him the Bionic man. His new valve could be heard
ticking away like a metronome.
On Saturday he was taken out of intensive care and moved to his own room where he spent the next couple of nights before
asking if he could leave the hospital and move back to the hospital apartment.
Dr Burke spoke with Peter and said it would be O.K.
 Peter, Dr Burke,Mom, Dad,Nicola and Katie-sue
Peter, Dr Burke,Mom, Dad,Nicola and Katie-sue
Peter made one return visit to M.C.H for his blood tests, his supply of Warfarin
tablets and to see if he was well enough to make the
return journey home. All was fine. A television crew hired via the B.B.C attended the hospital and interviewed the family and a
journalist who was interested in the case, took photographs and spoke about the case with the family and the surgeon.
The family started their journey home on the 12th August.
On arrival at Gatwick Airport the family were met by a photographer and a reporter from the Birmingham Evening Mail
who done an update on Peters success, they kindly transported the family back to Birmingham, where they were then greeted by Michele Paduano,
and a television crew from the B.B.C who then televised the interview.
Peter was now taking a daily dose of 4mg of Warfarin and was doing well.
A few days went by and Peter had just taken his medication when he vomited,
this became a problem as no one was sure whether he had kept the tablets down.
A telephone call was made to the hospital to check on the situation, they advised us to bring him in.
Unfortunately Peter had to spend the next fortnight on a ward before being discharged
as his I.N.R levels had dropped and this took 2 weeks to correct.
He now takes daily doses of Warfarin and the dosage varies between 6mg and 7mg.
Peters future treatment and well being needed to be addressed and Mom, Dad,
Peter and Peters cardiologist were invited to
attend a meeting with the Specialist Treatment Advisory Committee in December at which a decision would be made as to what
was best for him. It was agreed that Peter would best have his first annual evaluation
at Miami Childrens Hospital and that they would finance Peter + 1 adult to fly there.
Arrangements have now been made to return to Miami in September and all the family will travel together again covering the
extra costs themselves.
Regular trips are taken to the anticoagulation unit at Birmingham Childrens Hospital to keep his blood levels right.
Mom regularly takes to the Internet and through her experiences has helped other parents with heart children. She often
enters medical discussion groups, and as a result of visiting the G.U.C.H site (Grown Up Congenital Heart) was contacted
by Mr Michael Knight from Anticoagulation Europe, (a registered charity who provide information and advice to people on oral
anticoagulation therapy) who very kindly donated a Coagucheck machine to Peter,
which made him very happy.
This will benefit
Peter by enabling him to check his own levels more regularly and spend less time visiting hospital.
THIS STORY IS TO BE CONTINUED
Text by Lorraine - Graphics by DAUMAL Christian © 
| |
|
| |
|
|
|